According to a recent research, red blood cells are also important in the process of inflammation. When a patient has an infection such as malaria, sepsis, or a bacterial infection, they are more likely to develop acute inflammatory anemia. It is believed that red blood cells combat infection by scavenging mitochondrial DNA fragments that escape from wounded tissues. Why does a red blood cell transform from an oxygen-delivering cell into a disease-fighting machine, you may wonder? It has been a long time since we have understood why persons who are severely unwell with sepsis, trauma, COVID-19, a bacterial infection, or a parasite infection develop acute anemia.
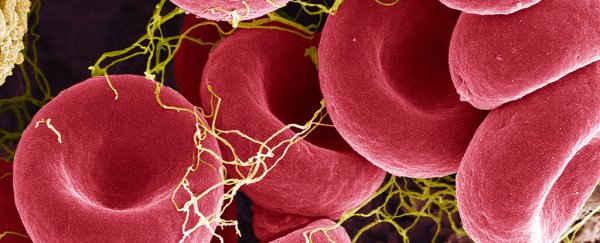
This engulfing triggers a chain reaction of inflammatory messengers, which effectively signals the immune system to respond in a time-sensitive manner. A higher level of mitochondrial DNA was found in mice infected with parasites as compared to red blood cells from non-infected animals, the researchers found. The standard practice currently in place when patients in the ICU [intensive care unit] become anemic, which occurs in almost all of our critically ill patients, is to administer blood transfusions, which has long been associated with a number of complications, including acute lung injury and an increased risk of death, according to Mangalmurti.
The induction of inflammation in areas of the body that are ordinarily not at risk of infection may be problematic, particularly in those who suffer from autoimmune illnesses.
Reference
Discovery Points to a Crucial Role Red Blood Cells Play in Our Immune Systems, https://www.sciencealert.com/red-blood-cells-play-a-much-greater-role-in-our-immune-system-than-we-thought?fbclid=IwAR0q44-OZClyDCcDJnNSCBluX9liisA_N0h8D9v7O9I2nghUU0LQNpli4KU
